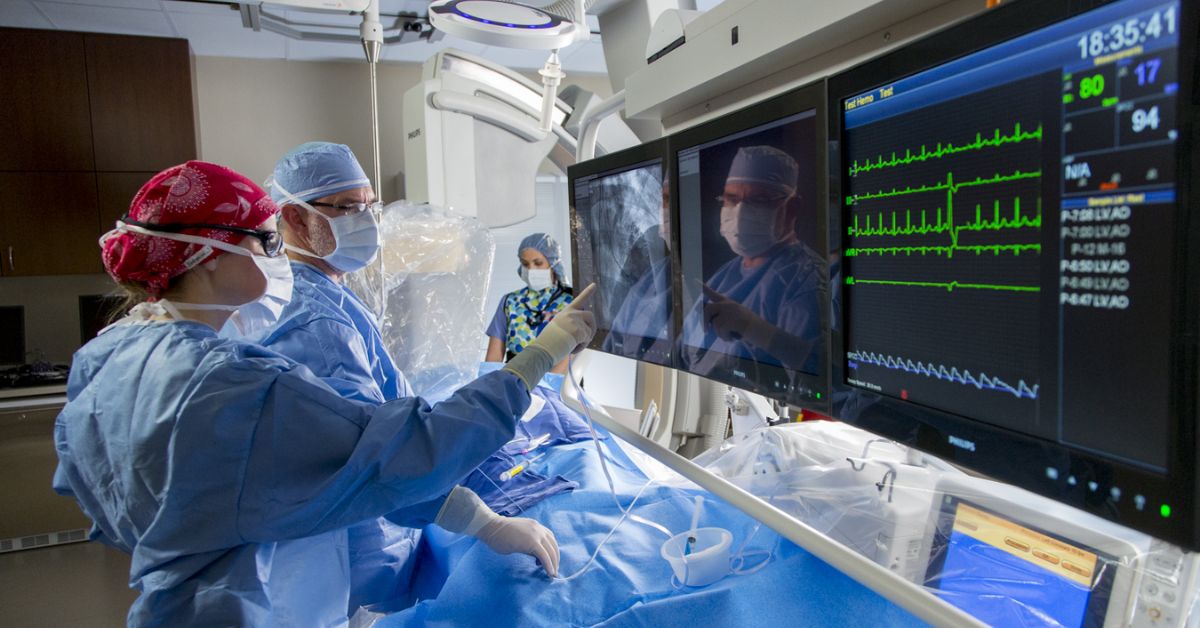
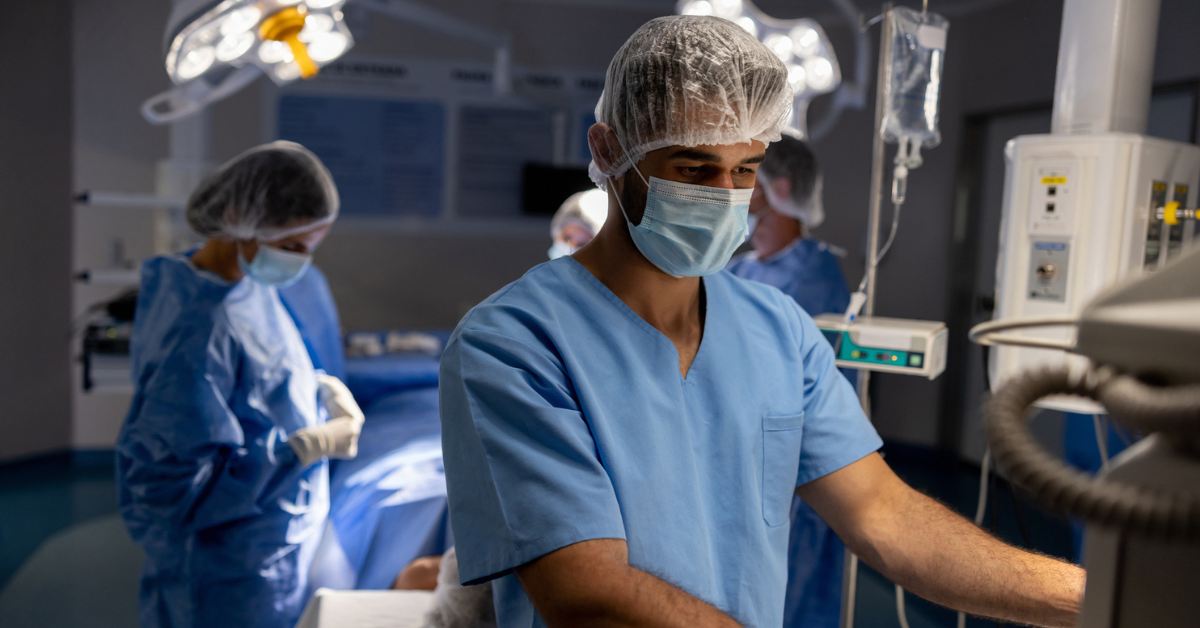
How to balance exceptional patient care & quality reporting
As more hospitals and health systems adopt value-based care, they are shifting to a more proactive approach to care delivery by placing emphasis on patient engagement, preventative care, and care management.
On top of that, healthcare organizations are also responsible for reporting performance data in the areas of quality, improvement activities, promoting interoperability, and cost.
 Although quality reporting and value-based care should work together, many organizations struggle to find success on both fronts simultaneously. When attempting to gather all of the necessary information for thorough quality reporting, providers can become overloaded and distracted during patient interactions.
Although quality reporting and value-based care should work together, many organizations struggle to find success on both fronts simultaneously. When attempting to gather all of the necessary information for thorough quality reporting, providers can become overloaded and distracted during patient interactions.
Not only does that negatively affect the patient experience, but it can also hurt the quality of care if a provider misses key information from the patient. As a result, hospitals and health systems are often pulled into a vicious cycle of trying to effectively report quality but missing opportunities to improve it in the process, and consequently falling short of achieving their goals.
The problem with today’s EHRs
Part of the reason it is so difficult to balance the two is that many of the programs used to manage patient care and reporting are behind the times. The professionals that use these programs are finding that the versions they use, many of which were created in the early 2000s, were not built to keep up with the changing healthcare landscape. From clunky interfaces to nonsensical layouts that require several clicks to navigate, many of the EHRs used today seem to interfere more than they help sometimes.
While these EHRs were designed with good intentions, the Centers for Medicare & Medicaid Services (CMS) has acknowledged the frustration they create and that upgrades are required to improve workflow for providers. In the meantime, this leaves hospitals and health systems searching for solutions to ensure that patient-centered care comes first.
Strategies for balancing reporting and patient care
Many are rolling out new strategies that make the best of what they have until the desired technology upgrades are available. Here are some examples:
- Identifying and leveraging templates or shortcuts that exist within the EHR
- Offering additional training and educational resources to improve expertise
- Hiring in-person or virtual medical scribes to manage workload
- Acknowledging and implementing potential process improvements
- Focusing on building and utilizing patient engagement skills
EHR programs that work for everyone are undoubtedly on the way. However, until they become a reality, it is important to seek and implement solutions that allow for a balance between effective reporting and quality patient care within your organization.
 company
company 
 (866) 755-7519
(866) 755-7519